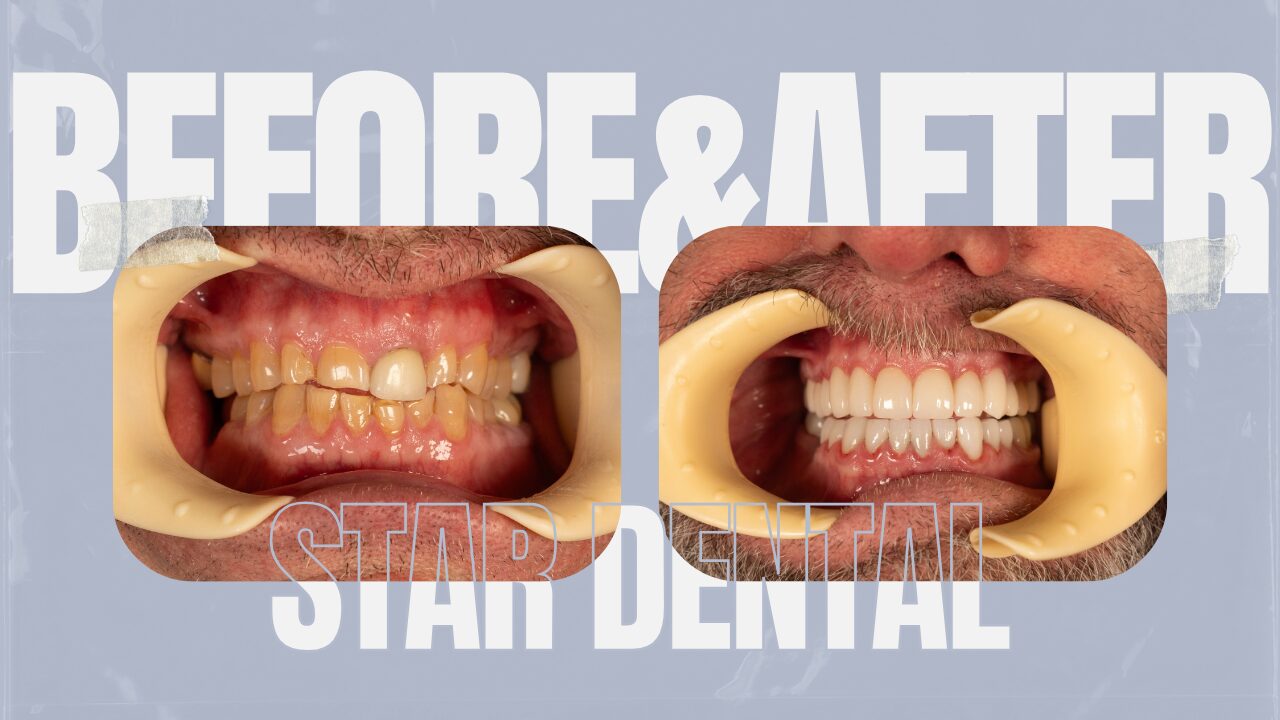
Restoration of Vertical Dimension in a Bruxism Patient with Obstructive Sleep Apnea
Introduction
Obstructive sleep apnea (OSA) is a multifactorial condition that often leads to secondary issues, including sleep-related bruxism and clenching, which in turn can cause a loss of dental vertical dimension.
In this case, chronic clenching and grinding led to tooth wear and shortening, disrupting both occlusion and overall facial balance. Restoring vertical dimension is critical not only for aesthetic improvement but also for reestablishing proper occlusal function and preventing temporomandibular joint (TMJ) discomfort. This case illustrates a comprehensive, interdisciplinary approach that integrates diagnostic measurements, digital 3D modeling, provisional testing, and adjunctive therapies to achieve a successful and stable outcome.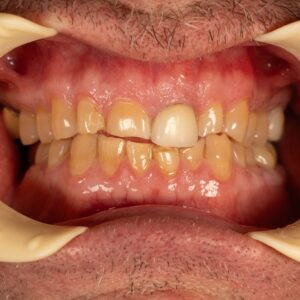
Case Presentation
The patient presented with a history of OSA and habitual clenching and grinding during sleep. Over time, excessive forces led to significant attrition, shortening the teeth and diminishing the vertical dimension of occlusion. This dental collapse was accompanied by concerns regarding potential TMJ pain and orofacial discomfort if a sudden increase in crown length was implemented without proper evaluation.
The patient’s OSA was diagnosed by a medical doctor, who also prescribed CPAP therapy to improve airway function and reduce sleep-related bruxism.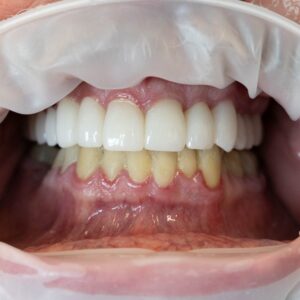
Treatment Protocol
Diagnostic Work-Up and Planning
- Comprehensive Measurements
- Detailed clinical measurements were taken to assess the patient’s lost vertical dimension. The focus was on ensuring that any restorative increase would not overstrain the TMJ or trigger facial pain.
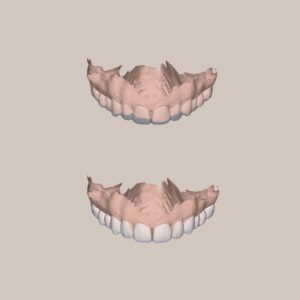
3D Modeling
-
- In collaboration with the dental laboratory, a 3D model was created based on the patient’s facial structure. Digital scans and facial records were used to design a model that accurately reflected the patient’s occlusal and aesthetic requirements.
Provisional Phase
- Fabrication of Temporaries
- Using the printed 3D model, provisional restorations (temporary crowns) were fabricated. The patient tried these temporaries for several weeks. During this phase, the occlusal changes were monitored closely, and the patient’s TMJ and masticatory muscles were evaluated for any onset of pain or dysfunction.
- Adjunctive Measures
- Recognizing that the underlying OSA was a primary driver of parafunctional habits, the patient was prescribed a continuous positive airway pressure (CPAP) device along with an oral appliance to support the airway during sleep. Furthermore, botulinum toxin (Botox) injections were administered into the masseter and temporalis muscles to relax the hyperactive muscles contributing to clenching.
Definitive Restoration
- Permanent Crowns
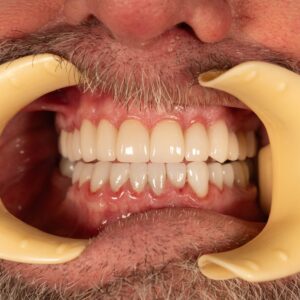
- After the trial period confirmed the patient’s tolerance, with no adverse TMJ or facial pain, the final permanent cosmetic crowns were fabricated and cemented. The new restorations successfully reestablished the vertical dimension and improved occlusion without compromising comfort.
Discussion and Analysis
This case underscores several key points:
- Gradual Restoration Is Essential
- Restoring vertical dimension in patients with a history of bruxism must be approached conservatively. By fabricating and trialing temporaries, clinicians can assess the patient’s adaptation to the new occlusal scheme. The absence of TMJ discomfort over several weeks provided confidence that permanent restorations would be well tolerated.
- Interdisciplinary Approach
- The successful outcome was achieved through collaboration between the clinician and the dental laboratory. Utilizing advanced digital workflows, such as 3D scanning and printing, allowed for precise replication of facial structures, ensuring that restorations were tailored to the patient’s unique anatomy.
- Addressing the Underlying OSA
- The use of CPAP and an oral appliance tackled the root cause of the bruxism. OSA is known to exacerbate clenching and grinding; by improving airway patency, these interventions reduced the frequency and intensity of parafunctional activity.
- Muscle Relaxation with Botulinum Toxin
- Botox injections into the masseter and temporalis muscles further contributed to symptom relief. Literature supports that botulinum toxin can effectively reduce muscular hyperactivity in bruxism patients, thereby protecting dental structures and reducing the risk of recurrent occlusal collapse.
- Preventing Future Relapse
- The combined approach—restoring tooth structure, managing occlusion, and treating OSA—created a stable environment that minimized the likelihood of recurrence. Ongoing use of the CPAP/oral appliance and periodic Botox treatments offered additional safeguards against the destructive cycle of clenching and grinding.
Conclusion
Restoration of the vertical dimension in a patient with OSA-related bruxism demands a carefully staged and multidisciplinary approach. In this case, diagnostic measurements, digital 3D modeling, and a provisional trial phase ensured that permanent restorations were implemented safely. Adjunctive therapies (CPAP, oral appliance, and Botox) addressed the underlying etiology and minimized the risk of future relapse.
This comprehensive treatment protocol not only reestablished functional occlusion and aesthetics but also exemplifies best practices for managing complex cases where sleep-disordered breathing intersects with dental wear and TMJ considerations.
This case serves as an excellent example of how digital planning and interdisciplinary treatments can restore dental function while protecting the TMJ in patients with multifactorial conditions like OSA and bruxism.